In today’s digital health landscape of 2026, the ability of wearable devices to anticipate clinical symptoms has reached levels of clinical precision. Understanding how a smartwatch detects fever and inflammatory states before a thermometer even records a temperature rise is crucial to fully leveraging these technologies. The smartwatch, the main entity of this hardware revolution, no longer limits itself to counting steps but acts as a true miniaturized diagnostic hub, constantly analyzing the fluctuations of our autonomic nervous system.
Biological Fundamentals: What the Algorithm Looks For
To understand how a wrist device can predict an illness, we must move away from the traditional concept of body temperature measurement. Predictive algorithms do not look for fever per se, but for the systemic immune response that precedes it. When a pathogen enters the body, the immune system activates hours, if not days, before evident symptoms like cough or fever manifest. This activation requires energy and alters the balance of the Autonomic Nervous System (ANS).
1. Heart Rate Variability (HRV)
Heart Rate Variability (HRV) is the king parameter in this field. HRV measures the time variation in milliseconds between one heartbeat and the next. According to official documentation from research institutes like Stanford Medicine, a high HRV indicates a relaxed and healthy body (parasympathetic dominance). Conversely, when the body fights an infection, the sympathetic nervous system (the «fight or flight» response) takes over. The result is a drastic drop in HRV. Modern smartwatches sample HRV during deep sleep to obtain data untainted by daily stress.
2. Resting Heart Rate (RHR)
Resting Heart Rate (RHR) is closely correlated with HRV. During the incubation of a virus, the basal metabolic rate accelerates to support the production of white blood cells and antibodies. This effort translates into an abnormal rise in RHR. If your historical resting heart rate is 60 bpm and suddenly, for two consecutive nights, it rises to 68 bpm without changes in training or alcohol consumption, the algorithm records a critical anomaly.
3. Skin Temperature and Respiratory Rate
The latest hardware sensors include high-precision skin thermometers (with deviations of 0.1°C) and algorithms for calculating respirations per minute (RPM). Nighttime skin temperature at the wrist is not equivalent to internal body temperature, but its deviations from baseline are very early indicators of inflammation. Similarly, an increase in nighttime respiratory rate is a strong predictor of lower respiratory tract infections.
Hardware Requirements: Necessary Sensors
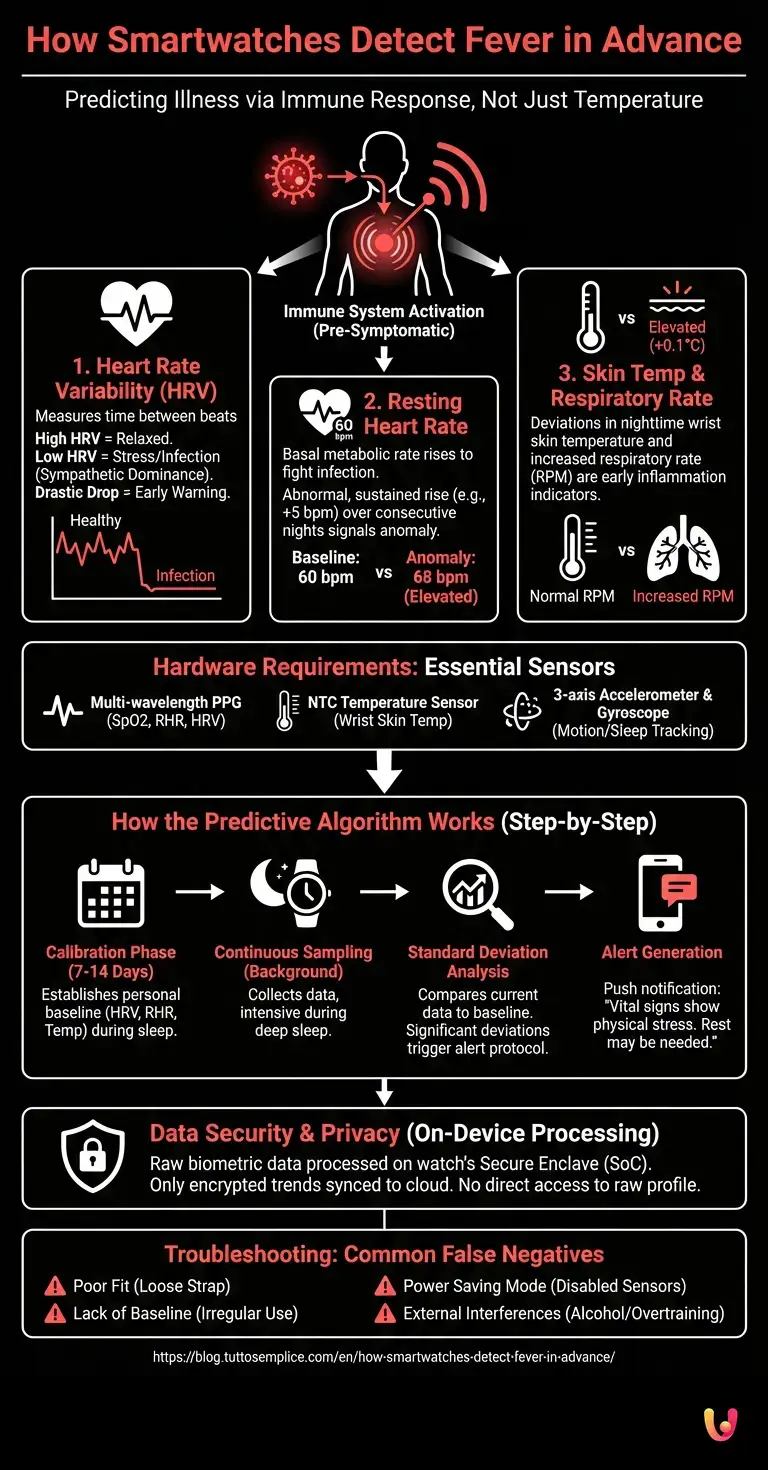
For the predictive algorithm to work, the smartwatch must be equipped with a specific suite of sensors. Not all devices on the market possess the adequate hardware:
- Multi-wavelength PPG Sensor (Photoplethysmography): Uses green, red, and infrared LEDs to measure microvascular blood volume and oxygenation (SpO2). It is essential for calculating RHR and HRV.
- NTC Temperature Sensor (Negative Temperature Coefficient): A thermistor placed in direct contact with the wrist skin, often accompanied by an ambient sensor to compensate for room temperature.
- 3-axis Accelerometer and Gyroscope: Fundamental for isolating biometric data from motion noise (artifacts) during sleep.
How the Predictive Algorithm Works (Step-by-Step)

The intelligence of these devices lies in the software. Here are the logical steps the smartwatch operating system performs to generate a potential illness alert:
- Calibration Phase (Baseline Establishment): When you wear the smartwatch for the first time, the algorithm requires 7 to 14 days of continuous use (especially at night) to establish your personal baseline. It learns what your normal HRV, RHR, and average temperature are.
- Continuous Sampling: The device collects data in the background. To save battery, intensive sampling (high frequency) usually occurs during deep sleep phases, identified via the accelerometer.
- Standard Deviation Analysis: The collected data is compared with the baseline. The algorithm uses statistical models (often based on lightweight neural networks running locally) to calculate standard deviations. A single anomalous night could be due to a heavy dinner; two consecutive nights with HRV dropping by 20% and RHR increasing by 5+ bpm trigger the alert protocol.
- Alert Generation: The system cross-references data (e.g., HRV drop + skin temperature rise). If the risk score exceeds a predetermined threshold, the user receives a push notification in the morning: «Your nightly vital signs show signs of physical stress. You may need rest.»
Data Security and Privacy (Hardware Level)
Dealing with sensitive health data, security is a fundamental pillar. As highlighted by GDPR and HIPAA regulations, raw biometric data should not be transmitted in plain text. Modern smartwatches use an On-Device Processing approach. The predictive algorithm runs directly on the watch’s chip (SoC), within a Secure Enclave. Only aggregated results (trends) are synchronized with the smartphone cloud, end-to-end encrypted, ensuring that manufacturers do not have direct access to the user’s raw health profile.
Troubleshooting: Why Didn’t the Device Detect the Anomaly?
Despite advanced technology, false negatives can occur. Here are the most common causes and how to resolve them:
- Poor Fit: If the strap is too loose, the PPG sensor cannot penetrate tissues uniformly, generating noisy data that the algorithm discards. Solution: Tighten the strap one notch before sleeping, positioning it two fingers away from the wrist bone.
- Lack of Baseline Data: If you reset the watch or do not wear it regularly at night, the algorithm does not have a reliable history to compare current data against. Solution: Wear the device 24/7 for at least two weeks.
- Power Saving Mode: Many battery-saving modes disable continuous background sampling of SpO2 and temperature. Solution: Ensure advanced sleep monitoring is enabled in the companion app settings.
- External Interferences (Alcohol or Overtraining): The algorithm detects physical stress but does not know what caused it. Extreme training or alcohol consumption depresses HRV exactly like a virus. In these cases, the device will signal an anomaly, but it is up to the user to contextualize it.
In Brief (TL;DR)
Modern smartwatches function as true diagnostic hubs, capable of predicting fever and illnesses by constantly analyzing the autonomic nervous system before symptoms.
These devices monitor crucial vital signs such as heart rate variability, resting heart rate, and skin temperature during deep sleep.
Advanced sensors and predictive algorithms establish a personal baseline, detecting abnormal deviations to generate timely alerts about potential ongoing inflammatory states.
Conclusions

The ability of smartwatches to act as early warning systems for diseases represents one of the most significant achievements of computing applied to health. By constantly monitoring parameters like HRV, RHR, and skin temperature, these devices manage to decode the silent signals of our immune system. While they do not replace an official medical diagnosis, they offer a valuable window of time to isolate, rest, and mitigate the impact of an impending illness. The future of wearable hardware will aim for increasingly less invasive sensors and even more specific predictive algorithms, perhaps capable one day of distinguishing between different types of pathogens.
Frequently Asked Questions

Wearable devices do not look for fever per se, but detect the body’s systemic immune response. By constantly analyzing vital signs such as heart rate variability, resting heart rate, and skin temperature during deep sleep, the software notes alterations in the autonomic nervous system. These variations manifest hours or days before the appearance of evident symptoms like cough or temperature rise.
The acronym HRV stands for Heart Rate Variability, which is the time variation between one heartbeat and the next. A high value indicates a relaxed body, while a drastic drop signals that the sympathetic nervous system is under stress to fight an infection. Modern smartwatches monitor this data at night to obtain precise measurements unaffected by daily stress.
False negatives can depend on several factors related to how the device is worn. The most common causes include a strap that is too loose preventing sensors from reading data correctly, a lack of baseline history due to occasional use, or having power saving mode activated. For effective monitoring, it is necessary to wear the device snugly and continuously.
Biometric data security is guaranteed by processing that takes place directly on the device chip, within a protected area. Only general trends are synchronized with the smartphone cloud via advanced encryption. This system ensures that manufacturing companies have no direct access to the person’s raw health profile, complying with strict privacy regulations.
When wearing a new device, the system requires a period of continuous use ranging from seven to fourteen days, focusing primarily on nighttime measurements. This calibration phase is essential to establish normal baseline values, such as resting heart rate and average temperature. Only after creating this history can the operating system accurately identify any deviations and generate health alerts.
Still have doubts about How Smartwatches Detect Fever in Advance?
Type your specific question here to instantly find the official reply from Google.
Sources and Further Reading

- Pre-symptomatic detection of COVID-19 from smartwatch data (National Center for Biotechnology Information)
- Heart rate variability and the Autonomic Nervous System – Wikipedia
- Heart rate variability and inflammation: A meta-analysis of human studies (NCBI)
- Photoplethysmogram (PPG Sensor Technology) – Wikipedia







Did you find this article helpful? Is there another topic you’d like to see me cover?
Write it in the comments below! I take inspiration directly from your suggestions.